High-grade masks evidence weak, Covid inquiry told
There is only “weak evidence” that high-grade face masks better protected health workers than surgical ones in the pandemic, the Covid inquiry has been told.
Prof Susan Hopkins, chief medical adviser at the UK Health Security Agency (UKHSA), said respirator masks – known as FFP3s – may have performed no better than thin surgical masks in real-life situations.
She said there could be “significant harms” from wearing tight-fitting FFP3s, including blisters and breathing difficulties.
“If the evidence was strong that FFP3s really protected people, and we saw a definitive reduction [in infections], they would have been recommended,” she said.
'Life and death'
Not all scientists agree on what has become a controversial issue.
The BBC has previously reported on research which appears to show a significant real-world benefit from wearing higher-grade masks on hospital wards.
Throughout the first two years of the pandemic, groups representing doctors, nurses and other health workers repeatedly called for urgent improvements to personal protective equipment (PPE), including the wider use of respirators.
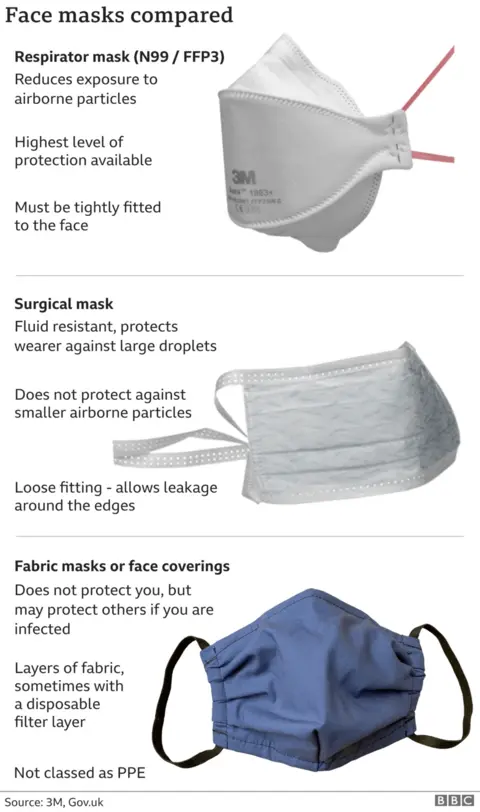
FFP3s are tight-fitting masks with a built-in air filter designed to block out tiny aerosol particles which can carry the virus.
Before they can be used, each wearer must undergo a fit test, to make sure the mask is properly sealed to the face.
For most of the pandemic, national guidance across the whole UK said that healthcare workers should wear basic surgical masks rather than FFP3s, except in intensive care or a small number of medical situations.
The decision was heavily criticised by some staff with the doctors’ union, the BMA, calling it a "matter of life and death".
National guidance on face masks from April 2020 was drawn up by a group of experts from across the United Kingdom known as the IPC (Infection Prevention and Control) Cell.
Its membership included representatives from the NHS, government departments and health bodies, including Public Health England (PHE), the organisation replaced by UKHSA in 2021 in a shake-up ordered by then-Health Secretary Matt Hancock.
The inquiry was shown minutes from an IPC Cell meeting on 22 December 2020, just after the new Alpha variant of Covid had been detected, which appeared to show disagreement about the use of higher-grade FFP3 masks.
The records quote Dr Colin Brown, now the deputy director of clinical and emerging infections at UKHSA but at the time with PHE, as saying: "Our understanding of aerosol transmission has changed. A precautionary approach to move to FFP3 masks [in all healthcare settings] whilst we are awaiting evidence should be advised."
However, the wider IPC Cell decided that no upgrading of the guidance was warranted at the time, and NHS trusts were told to continue to supply staff with standard surgical masks in almost all cases outside intensive care.
It was not until January 2022 that the advice changed, saying that FFP3 respirators should be available to "all relevant staff" depending on a risk assessment.
By that point, the World Health Organization, and other health bodies, had recognised Covid could be spread in tiny airborne particles over distances longer than 6.5ft (2m), something officials said was impossible at the start of the pandemic.
 Getty Images
Getty ImagesProf Hopkins, who served as PHE’s chief Covid adviser before moving across to UKHSA, told the inquiry that FFP3 masks offered a high degree of protection in laboratory studies, but the real-world benefits were less clear-cut.
“Where we looked at it, and repeatedly looked at it and are still looking at it, the evidence is weak that FFP3s protected more than fluid-resistant surgical masks,” she said.
“At the outset, in March 2020, the risks were that we had never asked people to wear FFP3 masks for prolonged periods.
“We saw them get ulcers on their faces and having challenges breathing and challenges in being hydrated.”
'Groupthink'
Asked about the December 2020 IP Cell minutes, which suggested PHE was pushing behind-the-scenes for the wider use of respirator masks in healthcare, Prof Hopkins said that was a "really challenging time" in the pandemic with the UK about to enter a third wave of the virus.
“The fact that PHE was giving and airing a different view is an example of [us] not being involved in groupthink,” she said.
The Covid inquiry is currently taking evidence about the impact on the NHS and healthcare systems across all four nations of the UK.
More than 50 witnesses are expected to appear in this third section or "module", which runs until the end of November.
